Ankyloglossia (Tongue Tie) and Oral Development
Who this is for
Parents who want a clear, calm explanation: what tongue tie means, how it may affect growth, and what you can do next.
Quick summary
Tongue tie (ankyloglossia) occurs when a tight or short band of tissue (lingual frenulum) under the tongue limits movement. That restriction can influence how a child feeds, breathes, chews, and speaks over time. Good news: with a collaborative plan and simple daily habits, you can support healthy function.
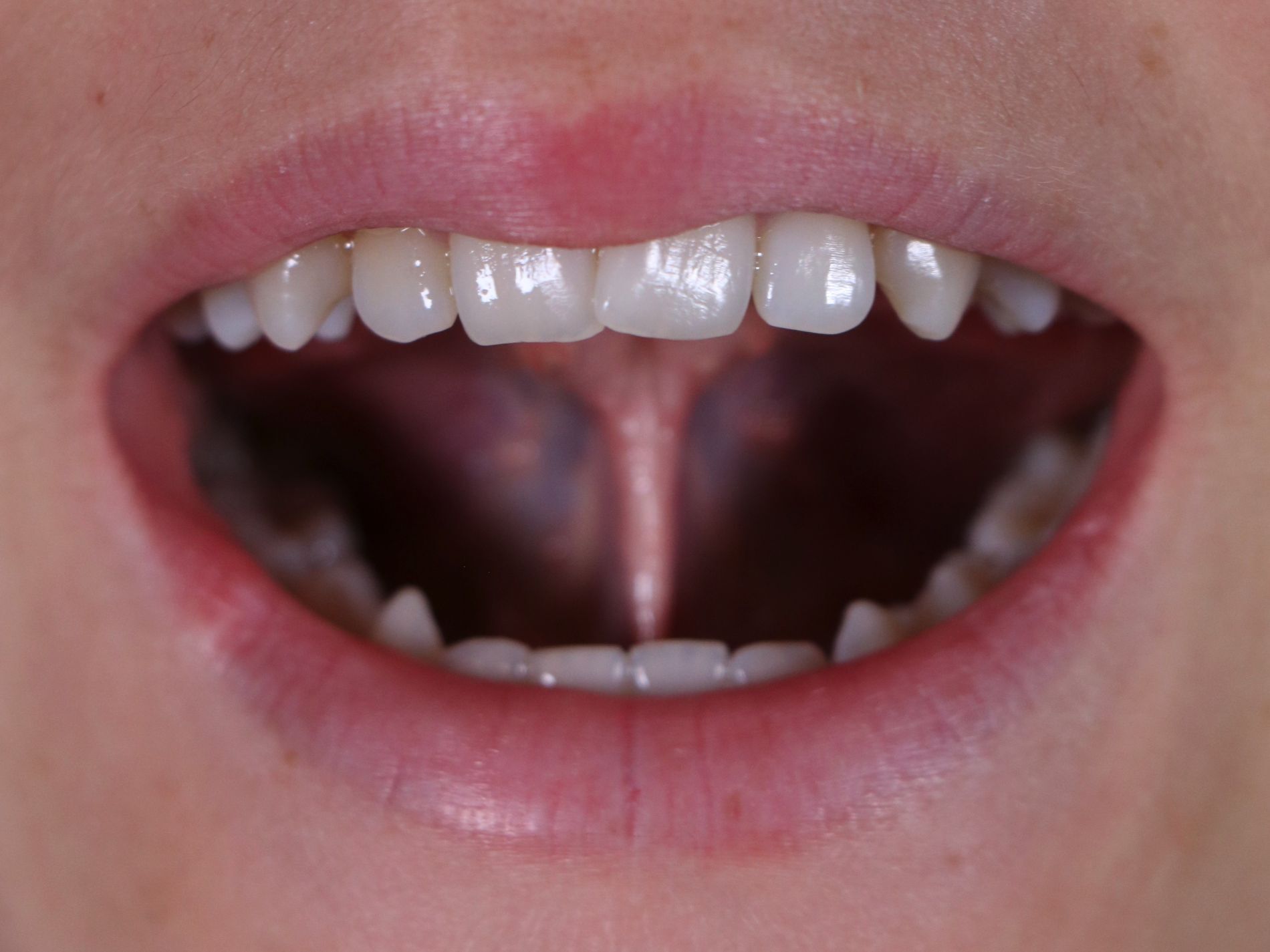
What is ankyloglossia?
The tongue is a powerful muscle that helps babies feed and kids develop strong oral habits. When the lingual frenulum is tight, the tongue may not lift, extend, or rest nicely against the palate. That limited range can change how a child uses their lips, tongue, and jaws day-to-day.
Key idea: function drives growth; small changes in daily muscle use can shape developing mouths.
Common signs parents notice
Not every child shows the same signs. Patterns to watch:
- Difficulty latching or prolonged feeds in infancy
- Frequent feedings and or inadequate milk transfer
- White, non-wipeable coating on the tongue
- Clicking sounds, dribbling, or fatigue during feeds
- Preference for soft foods, messy chewing, slow meals
- Open-mouth posture or mouth breathing at rest
- Restless sleep and or noisy breathing during sleep
- Low tongue posture; the tongue can't reach the palate
- Challenges with certain speech sounds as they grow
- Gummy smiles
- Recessed chin
- Dental crowding risks are tied to low tongue resting posture, weak lip seal, and underdeveloped jaws
These are mostly functional clues, not a diagnosis. A qualified practitioner will assess the oral development, structure and function together.
Why tongue mobility matters for development
Think of the mouth as a team: lips, cheeks, nerves, tongue and jaws working together.
- Feeding: Efficient latch and swallowing reflexes rely on palatal shape, tongue lift, and seal.
- Breathing: A tongue that rests up supports nasal breathing and a closed mouth.
- Chewing: Strong, rhythmic chewing activates facial muscles and supports jaw growth.
- Speech: Many sounds need precise elevation and control of the tongue tip and body.
Short lingual frenulum is associated with increased risk of sleep-disordered breathing in children. Recent systematic reviews show children with ankyloglossia have 3-fold increased odds of sleep-disordered breathing and 12-fold increased odds of high-arched palate. The mechanism involves tongue restriction limiting palatal development and promoting abnormal upper airway anatomy.[7]
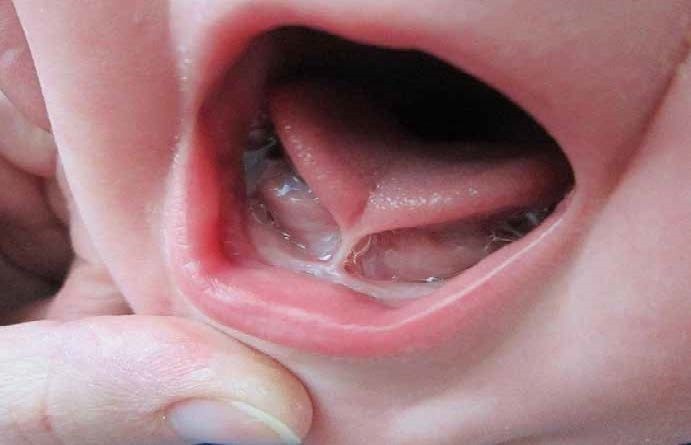
When movement is limited, kids often adapt and those compensations can keep less-helpful patterns in place.
Assessment: structure meets function
A thorough assessment looks at:
- Birth story including prematurity and any cranial / nervous system imbalances
- Shape of the palate
- Muscle tone
- Tongue appearance and movement
- Lip seal, nasal breathing, and resting posture
- Suck–swallow–breathe coordination
- Chewing pattern and endurance
- Whole-child factors like sleep quality and posture
Who can help?: Lactation Consultants, Dentists, ENTs, Osteopathic Physicians, Craniosacral Therapists, Speech Pathologists, Feeding Therapists, Specialty Chiropractors, Physical Therapists, Occupational Therapists, and Orofacial Myofunctional Therapy practitioners. A team approach protects your child's comfort and long-term function.
Treatment options: collaborative and conservative first
Every child is different. Many start with conservative care to improve function and oral development – especially tongue strength, lip seal and nasal breathing.
The American Academy of Pediatrics recommends infants start with lactation support and observation before considering surgical intervention. If a release (frenectomy) is considered, combining it with whole-body therapy, including non-surgical light laser therapy, may improve outcomes, though the evidence base is still developing. [1-2][4]
Research shows that surgery combined with neuromyofunctional re-education pre- and post-surgery may be more effective than either approach alone for improving tongue mobility and oral function in some children of all ages. However, these findings are based on a limited number of studies of varying quality, and more high-quality research is needed.[1][4-5]
Where Myo Munchee fits in – a supportive tool
Myo Munchee is a simple chew tool that may be used as part of neuromyofunctional retraining to assist oral development. While research on myofunctional devices specifically is limited, short, daily sessions are designed to help:[3]
- Increase tongue strength and endurance through patterned chewing and guided exercises
- Improve lip seal – lips together become the norm
- Support nasal breathing by reinforcing closed-mouth posture
- Encourage healthy jaw development by activating the muscles of mastication
Important to know: Orofacial myofunctional therapy and devices like Myo Munchee are emerging approaches with growing but still limited research support. Studies show promise, particularly when combined with other treatments, but most research to date has involved small numbers of participants and has varied in quality. These tools work best as part of a comprehensive plan guided by your practitioner.[1][3]
Daily habits that support oral function
Start small – consistency wins:
- Nasal hygiene: Clear the nose daily so nasal breathing is easy.
- Resting posture: Lips together, tongue up to the palate, teeth slightly apart.
- Chew practice: Age-appropriate foods that require chewing; slow down mealtimes.
- Myo Munchee sessions: Guided sessions to build endurance and awareness (if recommended by your practitioner).
- Screen-smart posture: Head up, mouth closed during screen time, feet parallel to the floor and supported.
Tip: Pair “Munchee” time with a routine: bath, story or homework; to make it stick.

FAQs for parents
Will my child "outgrow" a tongue tie?
Some children adapt, but restrictions can continue to influence function. A professional assessment helps you decide the next steps.
Does every tongue tie need surgery?
No. Many children benefit from observation and supportive therapy first. If a release is recommended, pre- and post-release therapy may support better outcomes, though research in this area is still developing.[1-2][4]
Is Myo Munchee a replacement for therapy?
No. It is one tool that may be part of a collaborative plan. Think of it as a daily "practice" that can reinforce new patterns, though more research is needed to understand its effectiveness fully.[3]
How long each day?
Your practitioner will set the plan. Many start with short, regular sessions and build endurance over weeks. A helpful resource for getting started can be found in the Myo Munchee Parent Checklist.
What does the research say about myofunctional therapy?
Current research suggests that myofunctional therapy may help improve oral function, particularly when combined with surgical treatment. However, most studies are small and vary in quality, and experts agree that more rigorous research is needed. The American Academy of Otolaryngology-Head and Neck Surgery notes that there is currently insufficient evidence to develop formal clinical practice guidelines for ankyloglossia treatment.[1][3-6]
Meet the Author

Dr Lynda Dean-Duru
Board-Certified Paediatric Dentist
Dentist Lynda Dean-Duru is a board-certified paediatric dentist who has devoted her career to advancing compassionate, integrative dental care for children and patients with special healthcare needs. With more than 20 years of clinical experience, she is recognised for her unique approach to functional and holistic paediatric dentistry, combining evidence-based care with innovative technologies and biologically informed treatment approaches.
She practises alongside her daughter, Doctor Krystle Dean-Duru, a board-certified paediatric dentist, at Ashburn Children’s Dentistry in Virginia. Together, they focus on airway-centred, growth-guided care that supports long-term oral health and overall well-being.
Doctor Dean-Duru practises at Ashburn Children’s Dentistry in Virginia, USA.
Websites: kidzsmile.com | womb2grow.com
Email: info@kidzsmile.com
Instagram: instagram.com/ashburnchildrensdentistry
Facebook: facebook.com/AshburnChildrensDentistry
Other Resources:
YouTube video: Ankyloglossia / Tongue Tie OMT and Myo Munchee Certified practitioner, Cathy Boyce, talks to us about ankyloglossia (tongue ties), how it can affect function and what to look out for. Always remember the 'why'!
References
1.Effectiveness of Myofunctional Therapy in Ankyloglossia: A Systematic Review.
González Garrido MDP, Garcia-Munoz C, Rodríguez-Huguet M, et al.
International Journal of Environmental Research and Public Health. 2022;19(19):12347. doi:10.3390/ijerph191912347.
Thomas J, Bunik M, Holmes A, et al.
Pediatrics. 2024;154(2):e2024067605. doi:10.1542/peds.2024-067605.
Practice Guideline
Shortland HL, Hewat S, Vertigan A, Webb G.
American Journal of Speech-Language Pathology. 2021;30(1):301-317. doi:10.1044/2020_AJSLP-20-00245.
Lichnowska A, Gnatek A, Tyszkiewicz S, Kozakiewicz M, Zaghi S.
Journal of Clinical Medicine. 2024;13(18):5354. doi:10.3390/jcm13185354.
Thornton AR, Montgomery EA, Graham ME, Riley CA, Lawlor CM.
Otolaryngology--Head and Neck Surgery : Official Journal of American Academy of Otolaryngology-Head and Neck Surgery. 2025;. doi:10.1002/ohn.1264.
New Reseach
6.Clinical Consensus Statement: Ankyloglossia in Children.
Messner AH, Walsh J, Rosenfeld RM, et al.
Otolaryngology--Head and Neck Surgery : Official Journal of American Academy of Otolaryngology-Head and Neck Surgery. 2020;162(5):597-611. doi:10.1177/0194599820915457.
7.Relationship of Ankyloglossia and Obstructive Sleep Apnea: Systematic Review and Meta-Analysis.
Camañes-Gonzalvo S, Montiel-Company JM, Paredes-Gallardo V, et al.
Sleep & Breathing = Schlaf & Atmung. 2024;28(3):1067-1078. doi:10.1007/s11325-024-03021-4.